Bunions FAQs
Bunions FAQs
written by Dr SW KONG
Last update: Aug 21st 2024
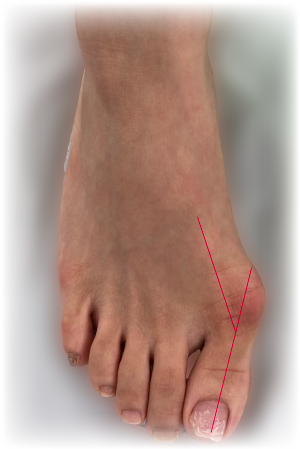
Fig. 1 Hallux Valgus |
What is Hallux valgus/Bunion ?
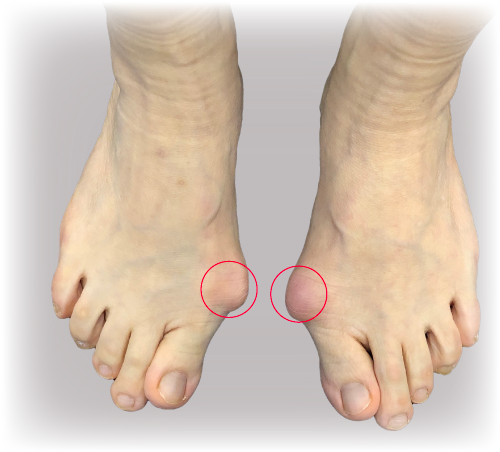
Hallux valgus (Fig 1) is the medical term for “bunions”. "Hallux" is the medical term for the big toe, and "valgus " refers to the abnormal angulation of the big toe towards the second toe. Usually, there is also a bump at the base of the big toe on the inner aspect of the foot, which is called a ‘bunion’ (Fig.2).
|
What causes Hallux Valgus/Bunions?
Hallux valgus is a biomechanical imbalance and occurs in about 2 - 4% of people. Most people have symptoms from 30 - 50 years old. There are various causes:
- Female gender: Hallux valgus is 15x more common in women than men.
- Family history: 58-88% of people have a family history.
- Other intrinsic conditions: flat feet, loose ligaments, abnormal bone structure, and certain neurological conditions.
- Extrinsic causes: Injuries; Narrow pointed-toe shoes; high heels etc
How does it affect me?
Mild Hallux valgus may not have symptoms except for the prominence of the bunion. Severe hallux valgus can lead to repeated inflammation and pain over the bunion where there is friction with shoe wear. As the bunion enlarges, there is increasing difficulty to fit into shoes. The second or other lesser toes may be deformed due to overcrowding and pressure, and they may have painful calluses on the sole. All these may make walking painful.
What is the natural history?
Hallux valgus usually gets worse over time.
How is Hallux Valgus/Bunion diagnosed?
History: Most patients complain of deformity and pain.
Examination: Review the combination of problems described above.
X-rays: Weight-bearing X-rays are usually sufficient to understand the problem (Figs. 3, 4 & 5).
Blood Tests: are sometimes needed if there is a suspicion of inflammatory arthritis (such as Rheumatoid arthritis).
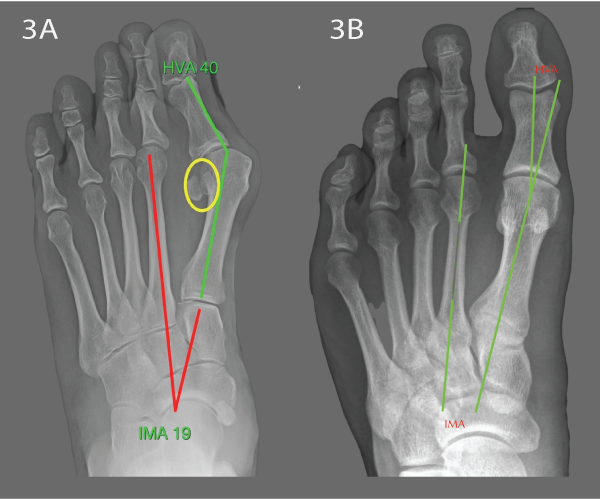
Fig 3a & b. Weight-bearing AP views of feet. Left: Hallux valgus. The angles HVA and IMA quantify the severity of the problem. The sesamoid bones have displaced from the normal position beneath the big toe (circle). Right: Normal for comparison. |
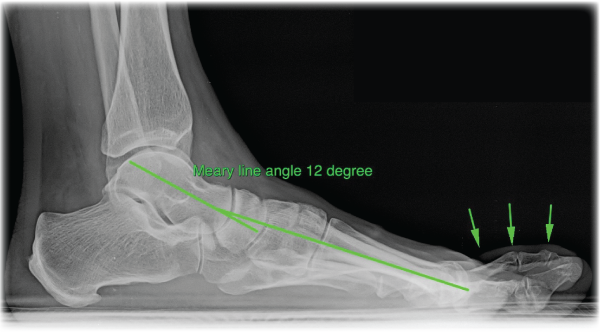
Fig.4 Weight-bearing lateral X-ray of the foot: The foot is flat. The Meary line angle quantifies the severity. The lesser toes are deformed (arrows) |
Fig.5 Classification of Hallux Valgus |
Could it be anything else?
The other common cause of pain and swelling at the base of the big toe is osteoarthritis of the joint, known as ‘hallux rigidus’. In hallux rigidus, the joint at the base of the big toe is usually painful and stiff, whereas in hallux valgus, the joint is deformed but usually not very painful. For information on Hallux rigidus, see the ‘Hallux Rigidus FAQs’. Sometimes, one can have both problems and in severe longstanding hallux valgus, the joint often develops osteoarthritis.
Pain at the base of the big toe is commonly diagnosed as gout, but confirming the diagnosis can be difficult. The only way to be absolutely sure is to take some joint fluid during an attack and examine it under the microscope for gout crystals. Often, patients labelled with ‘gout’ turn out to have ‘hallux rigidus’.
Athletes with bunions can develop pain because of stress fractures and other problems. Because one has bunions it does not mean the bunion is automatically the source of any pain in the foot – new pains should be properly assessed.
Bunion Treatment options?
In mild cases, symptoms can be improved by adjusting shoes – such as wider shoes, soft materials, possibly custom-made shoes, and, as much as possible, avoiding very high heels. This may slow down the deterioration of the condition, but usually, it does not completely stop the progress.
Moderate deformity cases may be helped with the addition of ‘orthotics’. A Hallux valgus splint for night-time stretching helps to slow down progress, a spacer/spreader between the big toe and the second toe helps to avoid friction during the day, and a custom-made arch support insole, made by a podiatrist, can correct any associated flat feet. Claw toe splints can help to prevent lesser toes rubbing on shoes. Whilst orthotics can be helpful, they are not very convenient and do not ‘cure’ the problem – they only help to relieve symptoms while they are worn but cannot permanently correct the deformity.
Cases with severe deformity and intractable symptoms or failure of orthotic treatment are best treated by an operation. Surgery is the only method to permanently correct hallux valgus, by correcting the deformity and rebalancing the toe. Most surgeons would recommend surgery only if a patient had pain and functional disability, and not simply for cosmetic reasons, though the foot will look much better afterwards.
What kind of operation should I have?
There are more than a hundred and thirty different hallux valgus surgeries described in the medical literature, but no single surgery has proved itself to be the best. However, most modern surgeries have the same underlying principle: to ‘rebalance’ the toe by correcting all the deformities and making the foot as biomechanically normal as possible. The exact surgical procedure depends on an individual’s particular problem.
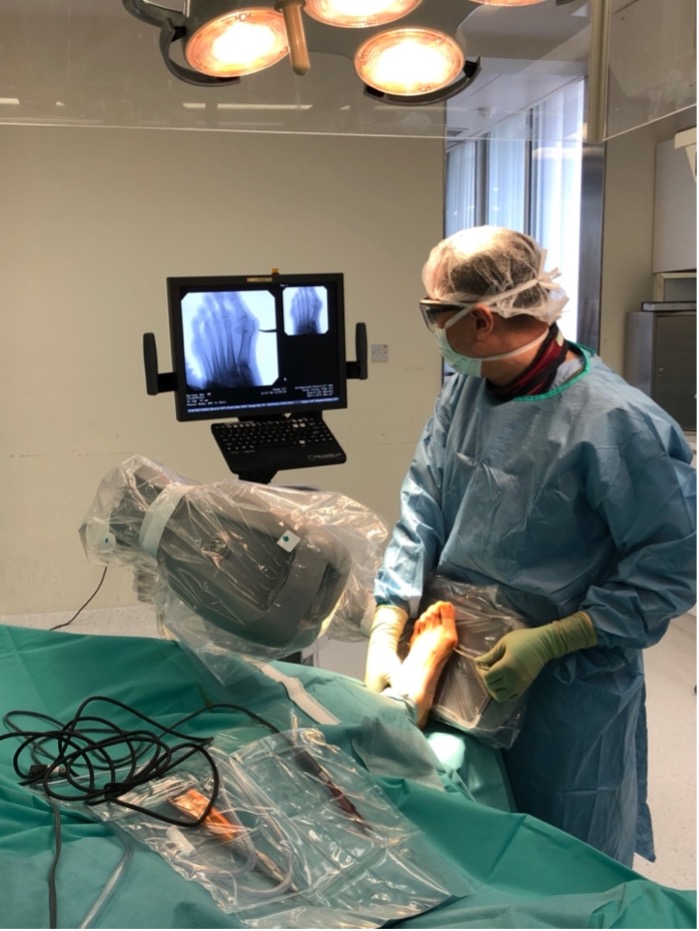 Fig. 6 Minimally invasive surgery using a fluoroscope |
Can I have a minimally invasive approach?
In some cases, new techniques are promising. If a' minimally invasive approach' is possible to achieve the primary goal of fully correcting the deformity and rebalancing the toe, we do so, but we do not compromise the operation (and thus the result) for the sake of a slightly shorter scar. A minimally invasive approach has the advantage of causing minimal injury to adjacent tissue and leading to a faster post-operative recovery rate.
Surgery is now generally possible with a minimally invasive approach for mild to moderate bunions and selected severe bunions (1,2). However, an open approach with a larger incision is usually recommended for more severe cases.
The surgery is performed through a small incision using a fluoroscope (a video X-ray) to show the bones (Fig 6).
Different Types of Bunion Operations
Whether via a minimally invasive or conventional approach, in most cases we use ‘Chevron osteotomies’ in the 1st metatarsal bone, and, if necessary, the bone at the base of the big toe (the proximal phalanx), to realign the toe. Screws are then inserted to hold the cut bones in the corrected alignment (Figs 7 & 8).
 |
| Fig.7: Imaging of a planning path of Chevron Osteotomy, Realignment of bones and Screw fixation |
 |
| Fig.8: Imaging of before and post-surgery of Chevron Osteotomy, Realignment of bones and Screw fixation |
For people with multiple deformities beside the big toe, then more extensive surgery to correct all deformities will be needed.
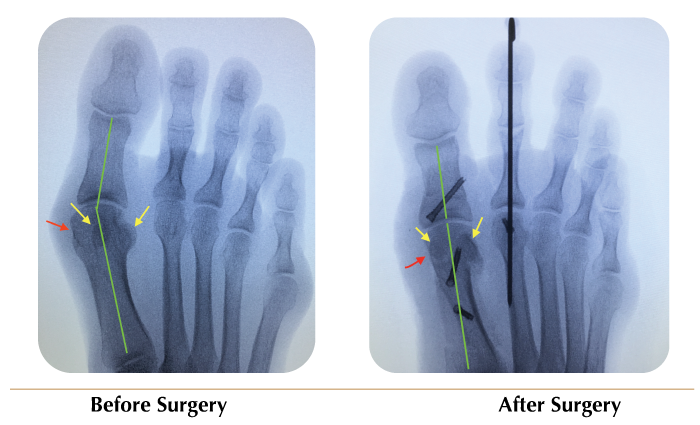
- Bunion: The bone forming the bunion is usually cut off with a saw. Removal of the bunion is called ‘bunionectomy’ (Fig 9a-b).
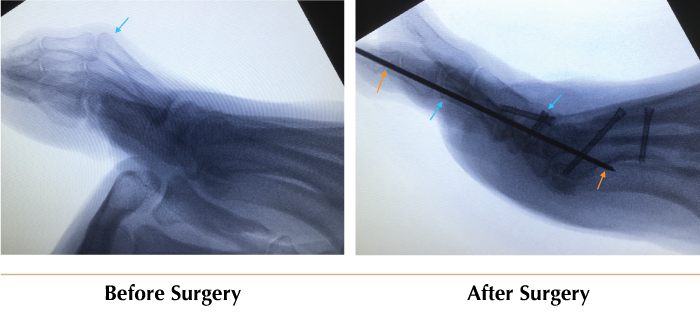
- Lesser toe deformities: The toes are straightened so they no longer rub on shoes or jam on the floor (Fig 9c-d).
- Bunionettes: If a bunion of the little toe (called a ‘bunionette’) is causing problems, this can be corrected with a small osteotomy of the 5th metatarsal at the little toe.
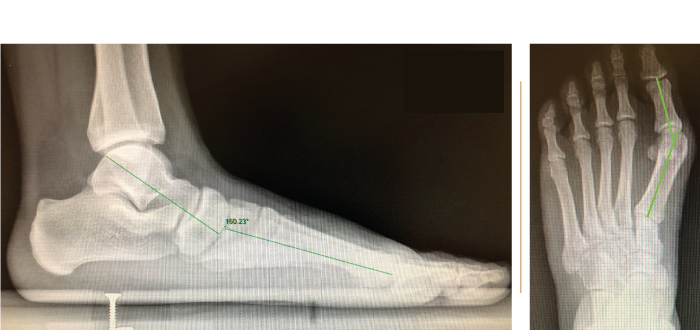
- Flat foot: Flat feet may also contribute to the problem of bunions (Fig 10), so it is often helpful to correct them too. Our preferred correction methods include:
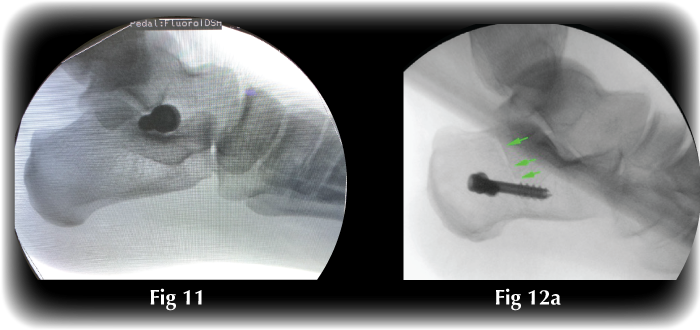
- Arthroeresis is a procedure to control motion in the subtalar joint, which will correct the flat foot deformity (Fig 11).
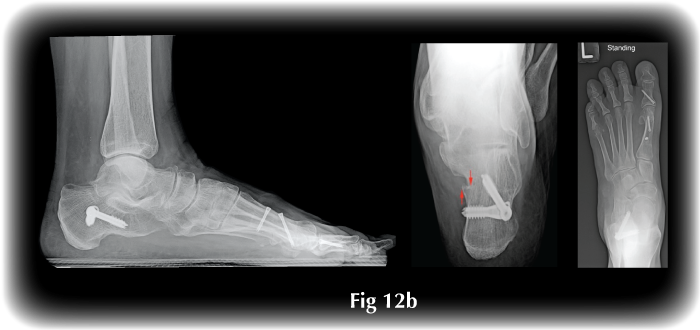
- Calcaneal Osteotomy is a procedure to cut and translate the heel bone and then fix it with buried screws in order to correct the hindfoot mal-alignment and, thus, the flat foot (Fig 12).
The red arrow shows the site of the bunion, which is removed. Osteotomy of bone corrects the HVA angle (green lines). Yellow arrows show the sesamoid bones, which are malpositioned pre-surgery and in the normal positions post-surgery. |
Fig. 9c-d Lesser toe deormities Same patient as Fig 9a has concomitant lesser toe deformity (blue arrow), which is fixed, the metal pin (orange arrows) will be removed in the office at 6 weeks post-surgery. |
Fig. 10 Weght-bearing X-rays showing Hallux valgus associated with flat foot |
Fig. 11 ‘Arthroeresis’ procedure to treat flat foot by fixing the foot in a corrected position. Fig 12a: Calcaneal osteotomy (green arrows) is fixed with screws, correcting the flat foot |
|
What will my feet be like?
Most people are delighted with the result of the operation, as their foot looks normal (Fig 13), they can wear normal shoes, and usually pain goes away. The big toe resumes its normal job actually helping one to walk further and faster. One can return to sport. Most people go on to have the second foot operated as they are pleased with the result of the first foot.
Fig 13:Appearance of the foot after minimally invasive bunion surgery. Red arrows show the surgical scars. |
Fig. 14 DARCO boot |
What does operation involve?
Hallux valgus operations are performed in the hospital operating room. Usually, we anaesthetise the foot by injecting local anaesthetic around the ankle – this is called an ankle block, and it lasts for a few hours after the operation, thus providing excellent post-operative pain control. It is possible to perform the surgery with an ankle block alone. Still, we also usually use a tight tourniquet around the thigh to prevent bleeding during the operation. The tourniquet can be uncomfortable, so we recommend additional light anaesthesia – either a light general anaesthetic or a spinal or epidural anaesthetic, as-well-as, or in-place-of, the ankle block, and, with this anaesthetic, one can be awake or asleep during the procedure. The operations take from 45 minutes up to 2 hours, depending on what is required. Incisions are made in various places as required, the operation is performed to correct the deformities, the incisions are stitched closed (usually with invisible dissolving sutures). One goes home with the aid of crutches and a special shoe - we typically recommend a DARCO boot (Fig 14).
What happens after the operation?
Physiotherapy helps to make one feel more comfortable, to walk more easily and to regain strength and flexibility of the foot. One walks with the special shoe for 6 weeks, then loose ordinary shoes, and most people switch back to normal or dress shoes at 12 weeks, but we advise avoiding very narrow, very high-heeled shoes, as these are likely to increase the rate of recurrence. We recommend saving such shoes for parties!
When can I return to work?
This depends on the type of surgical procedure, one’s occupation and the accessibility of one’s place of work. Usually, it takes 3 weeks to 3 months, depending on one’s job.
If one can work at a desk with one’s foot up, use crutches at work, and take breaks as needed, one can return to work in as little as one week. If one needs to stand for long periods and be physically fit to work, for example, as a police officer or flight attendant, it will more likely be 3 - 6 months before one can return to normal duties.
Can I have both sides done together?
For relatively simple bunions, one can consider having both feet operated at the same time. However, we do not recommend this for those who need more complicated procedures. Please discuss this with your surgeon.
What are the risks of a bunion operation?
- Anaesthesia: There is a small risk of complications associated with an anaesthetic, though modern anaesthesia is very safe.
- Surgical risks are divided into general risks, which can occur in any operation, and specific risks of hallux valgus surgery.
- General risks include: a small risk of infection; a clot (deep vein thrombosis or ‘DVT’) possibly leading to a serious pulmonary embolus; and others. General complications are uncommon in foot and ankle procedures [2].
- Specific risks:
- Swelling: It is normal for the foot to be quite swollen for about 3 months and for it to take a full year for the foot to return entirely normal. This is not a complication, it is a normal result of gravity.
- Stiffness: This may occur due to the initial period of immobilisation. Once the tissues are healed the physiotherapists will supervise stretches.
- Under-correction or recurrence: There is no clear guideline for what constitutes a ‘standard’ result, as the results can vary with the severity of the deformity, the extent of soft tissue rebalancing required as well as the site and extent of any bony correction. Recurrences are not common, and depend to a large extent on one’s choice of shoes.
- Over-correction: There is a small chance of correcting too much and producing ‘hallux varus’ with the big toe deviating inward. This is mostly a cosmetic issue, but could require repeat surgery. Documented incidence is 1-3% [3].
- Avascular necrosis: Loss of blood supply to the bone leading to bone death, causing pain and other problems. This is uncommon and has become less common since the modification of soft tissue release procedures [4].
- Pain: It is normal for one’s feet to be quite uncomfortable for a few weeks, but very occasionally one may experience unusually severe pain due to nerve ‘overreaction’ – this is known as ‘causalgia’ or ‘complex regional pain syndrome’ and may require treatment by a pain specialist.
- Nerve damage: It is common to get a little numbness or pins & needles near to the incisions due to damage to small nerves in the skin. This does not usually worry people. The use of a tourniquet (to provide a bloodless surgical field) sometimes causes numbness due to the nerve compression, which usually recovers within 2 – 3 days, however individuals with underlying nerve degeneration, such as in diabetes, could have more severe problems. Very occasionally there is damage to a larger nerve resulting in numbness of a larger area of the foot – this can be unpleasant - annoying or disturbing - but is not usually a serious problem [5].
- Implant problems: If an implant, such as a screw, is used, various problems, including skin impingement, loosening, breakage, or infection, may occur. If so, the implant may need to be removed – this is usually a very minor procedure with a very quick recovery. There is no need for routine implant removal. Most of the implants are buried entirely in the bone, cannot be felt, and can safely remain in place for life.
Is there anyone who should not have hallux valgus surgery?
Individuals who are unable to cope with the demands of the rehabilitation.
People who are not very healthy, for example with medical problems such as heart disease, are at higher risk of complications, and it would be necessary to carefully weigh the risks and benefits.
People with poor blood supply to the feet are at greater risk, and it would be necessary to carefully weigh the risks and benefits.
Diabetes is not an absolute contraindication for surgery, but it would be necessary to carefully weigh the risks and benefits.
Active infection in the foot is an ‘absolute contraindication’ – it would need to be treated first.
What about children?
This is not an absolute contraindication, as significant hallux valgus can occur in quite young people, but in general we advise delaying until skeletal maturity, usually around 13 years of age, if possible. One example of child had Xray done at eight years old (Fig.15a) and another xray after skeletal maturity at 14 years old(Fig.15b), there is deterioration in severity and we will do surgery after skeletal maturity reach.
Fig 15:(Left) Imaging when the child is 8 years old, (right) when the child is at 13years old |
References
- Lam Ka Lee Karry, SW Kong et al Percutaneous Chevron Osteotomy in Treating Hallux Valgus: Hong Kong Experience and Mid-term result Journal of Orthopaedics, Trauma and Rehabilitation xxx (2015) 1-6
- Thalava, R. and R. Thalava, Venous thrombosis after hallux valgus [comment]. Journal of Bone & Joint Surgery - American Volume, 2004. 86-A(4): p. 872; author reply 872.
- Sammarco, G.J. and O.B. Idusuyi, Complications after surgery of the hallux. Clinical Orthopaedics & Related Research, 2001(391): p. 59-71.
- Shariff, R., et al., The risk of avascular necrosis following chevron osteotomy: a prospective study using bone scintigraphy. Acta Orthopaedica Belgica, 2009. 75(2): p. 234-8.
- Tarver, H.A., et al., Techniques to maintain a bloodless field in lower extremity surgery. Orthopaedic Nursing, 2000. 19(4): p. 65-73.
| Copyright ©2021 Asia Medical Specialists Limited. All rights reserved. |