Sacroiliac Joint Pain FAQs
Sacroiliac Joint Pain FAQs
Written By DR CHOW Hung-Tsan
(Last updated on: September 15th 2020)
Sacroiliac (SI) joint pain is a challenging condition affecting 15% to 25% of patients with axial low back pain, for which there is no standard long-term treatment. Recent studies have demonstrated that historical and physical examination findings and radiological imaging are insufficient to diagnose SI joint pain. The most commonly used method to diagnose the SI joint as a pain generator is with small-volume local anesthetic blocks. In the article, I will try to explain the diagnostic methods and available treatments in detail.
Structure and Function of the SI joint
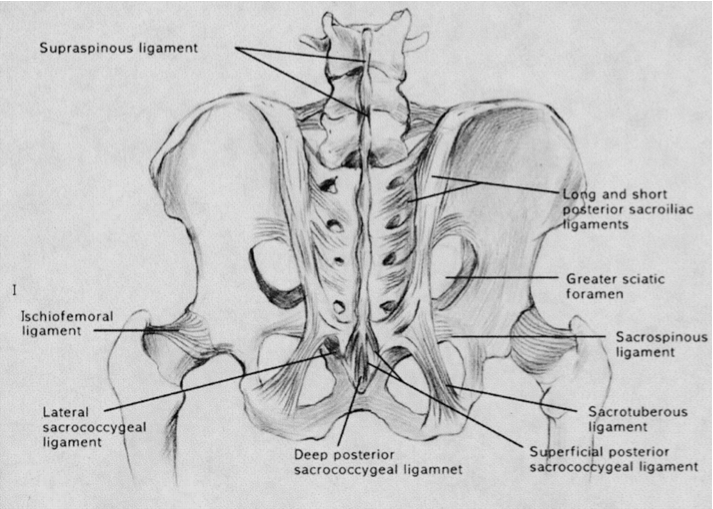
The sacroiliac joint is the largest axial joint in the body, with an average surface area of 17.5 cm [1]. There is wide variability in the adult SI joint [2, 3]. The SI joint is most often characterised as a large, auricular-shaped, diarthrodial synovial joint. It has no joint capsule at the posterior and is covered by an extensive ligamentous structure, functioning as a connecting band between the sacrum and ilia. The ligaments are serving a static stabiliser to the joint. (Fig. 1) In addition, the SI joint is also supported by a network of muscles (gluteus maximus, piriformis and biceps femoris) that help to stabilise the pelvic bones.
Fig. 1 Posterior ligamentous structures stabilizing sacroiliac joint. |
Normal Aging of SI joint
Age-related changes in the SI joint begin in puberty and continue throughout life. Degenerative x-ray changes are usually found by the third and fourth decades. In the sixth decade, motion at the joint may become markedly restricted as the capsule becomes increasingly rigid.
Nerve supply to SI joint
The innervation of the SI joint remains a subject of much debate. Some authors have suggested that the anterior SI joint is devoid of nervous tissue [4, 5]. However, it is commonly believed that the lateral branches of the L5-S3 dorsal rami are responsible for the major nerve supply to the posterior SI joint [1].
Prevalence
Bernard and Kirkaldy-Willis, who performed the largest prevalence study, found that 22.5% of patients presenting with low back pain were suffering from SI joint pain [6]. By using criteria based on International Spinal Injection Society guidelines [7], the prevalence of SI joint pain in carefully screened LBP patients appears to be 15%–25% [8].
Causes of SI joint pain
Can be divided into intra-articular and extra-articular causes.
Intra-articular causes - arthritis and infection
Extra-articular causes - enthesopathy, fractures, ligamentous injury, and myofascial pain.
The mechanism of SI joint injury has is a combination of axial loading and abrupt rotation. This injury can lead to capsular or synovial disruption, capsular and ligamentous tension, hypomobility or hypermobility, extraneous compression or shearing forces, abnormal joint mechanics, microfractures or macrofractures, chondromalacia, soft tissue injury, and inflammation [9].
Factors affecting SI joint pain
Risk factors that operate by increasing the stress borne by the SI joints include:
1. pregnancy
2. true and apparent leg length discrepancy
3. gait abnormalities
4. prolonged vigorous exercise
5. scoliosis, and spinal fusion to the sacrum
Diagnosis and Presentation
History and Physical Examination
One of the most challenging aspects of treating SI joint pain is the complexity of diagnosis. Questions will be asked to differentiate the other pathologies such as lumbar disc disease, nerve root compression, facet joint pain, primary or secondary myofascial syndromes, and symptoms from nonspinal structures all may mimic sacroiliac joint pain. Inflammatory disorders of the sacroiliac joint, including ankylosing spondylitis and Reiter's syndrome, often are diagnosed clinically.
Physical examination should include a thorough neurologic examination with evaluation of straight leg raising and assessment of pain and motion loss throughout the lower thoracic and lumbar spine. The hip joint should be tested and palpated for focal zones of soft-tissue or osseous pain in the lumbosacral pelvic region. The patient should point to the area of maximal pain, and its location should be noted. Focal areas of tenderness along the sacroiliac joint line and in the sacral sulcus is a typical sign.
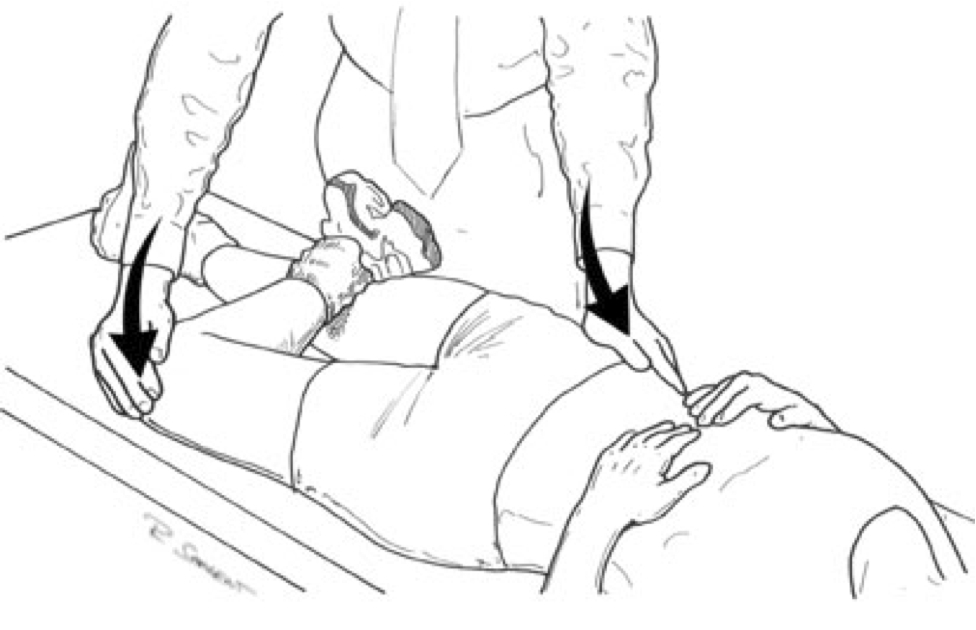
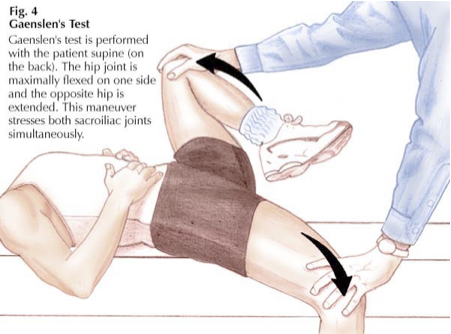
In the literature, there are plenty of physical signs or tests for detecting SI joint pain. Patrick's test (Fig. 2) and Gaenslen's test (Fig. 3) are the 2 commonest physical examinations [10]. The reliability of provocative SI joint manoeuvres and alignment/mobility tests are not well validated.
|
Fig. 3 Gaenslen's test to stress the sacroiliac joint by full flexion of hip joints. |
Radiological Studies
Plain radiographs for confirmation of the pathology of the SI joint pain are very disappointing. MRI and CT scan can produce a better image of the architecture of the joint. They are reportedly 57.5% sensitive and 69% specific in diagnosing SI joint pain [11]. Radionuclide bone scanning in the identification of SI joint pain has sensitivity of 46% [12].
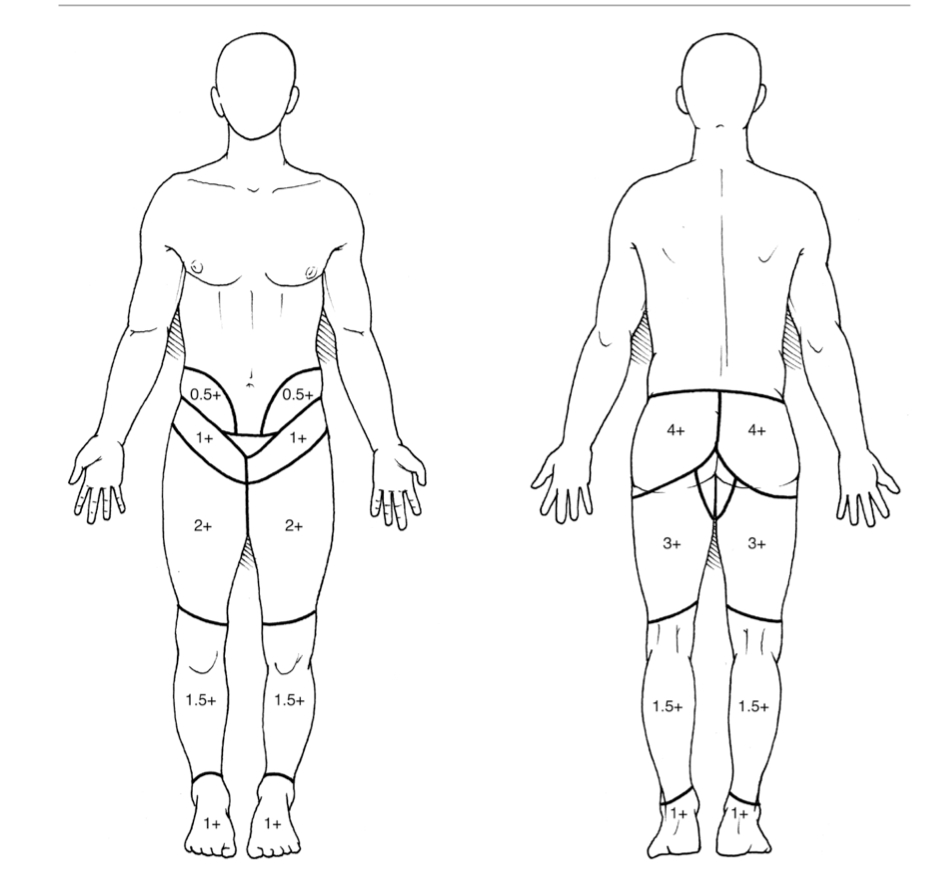
Pain Referral Patterns (Fig. 4)
• Sensory changes are localised to the medial buttock inferior to the posterior superior iliac spine, the superior aspect of the greater trochanter and the upper thigh.
• Pain referral patterns for SI joint pain are buttock (94%), lower lumbar region (72%), calf (28%), groin area (14%), and foot pain (12%). Radiating pain to upper lumbar region (6%), and abdomen is rare (2-6%) [13-15].
Fig. 4 Pattern of radiation of SI joint pain to the limbs. |
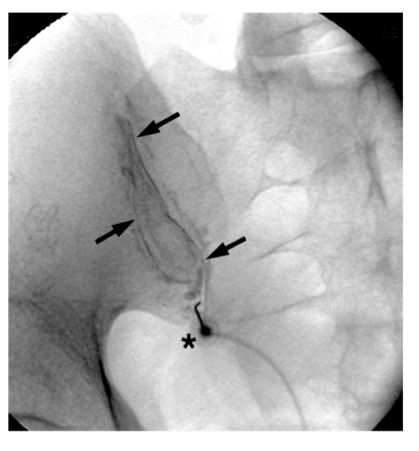
Diagnostic Blocks (Fig. 5)
Diagnostic block is the most reliable method to diagnose SI joint pain. The current standard is X-ray guided injection. Sometimes, CT guidance is necessary because of technical difficulty. Failure rate is around 5% with fluoroscopically guided SI joint injections [16,17].
Limitation of diagnostic block includes the placebo effect, convergence and referred pain, neuroplasticity and central sensitisation, expectation bias, unintentional sympathetic blockade, systemic absorption of local anaesthetic, and psychosocial issues [18].
|
Treatment
The treatment of SI joint pain is well established. In general, the treatments can be divided into 2 categories:
1. directed at correcting the underlining pathology
2. aimed at alleviating symptoms
Conservative Management
The non-interventional management of SI joint pain should ideally address the underlining pathology.
Correct underlying factors such as leg length discrepancy. Physical therapy and osteopathic or chiropractic manipulation can reduce pain and improve mobility [19]. Ankylosing spondylitis (AS) and other seronegative spondyloarthropathy should be treated with immunosuppressant medicines by a rheumatology specialist.
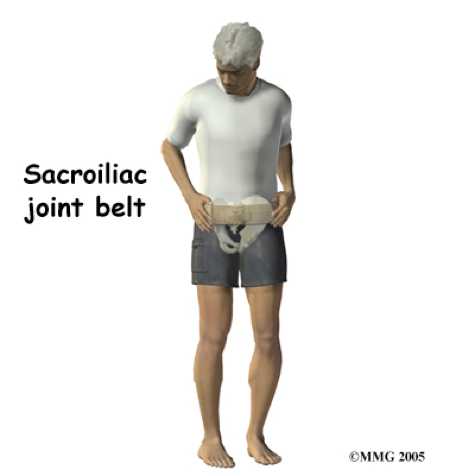
Nonsurgical stabilisation programmes such as application of pelvic belts (Fig. 6) and exercise-induced pelvic stabilisation programs are effective in many cases [20, 21].
Fig. 6 Sacroiliac joint belt for external support of sacroiliac joint instability. |
Hyaluronic acid injection
A viscosupplement to the joint. By injecting this substance, the joint may have a chance to recover. The initial results are promising but the counterpart studies in the knee joints have shown weak evidence in providing a good long-term pain relief. In addition, degenerative SI joint disease accounts for only a small percentage of patients [22]. Therefore, it is not a commonly used method.
Proliferative therapy (a.k.a. "prolotherapy")
It has been advocated as a treatment for nonspecific low back pain and SI joint pain. The rationale behind the use of "prolotherapy" is that the ligaments and other soft tissue structures are of primary importance in the development of low back pain. Thus, the injection of a drug promoting fibroblast hyperplasia should theoretically increase the strength and reduce sensitisation of these structures. In the literature, there is no evidence showing that the prolotherapy can generate a long-term success in reducing the pain [23].
Steroid injections
Injections with steroid and local anaesthetics often serve the dual function of being therapeutic and aiding in diagnosis. X-ray guided SI joint injections provide good to excellent pain relief lasting from 6 months to 1 year [24,25].
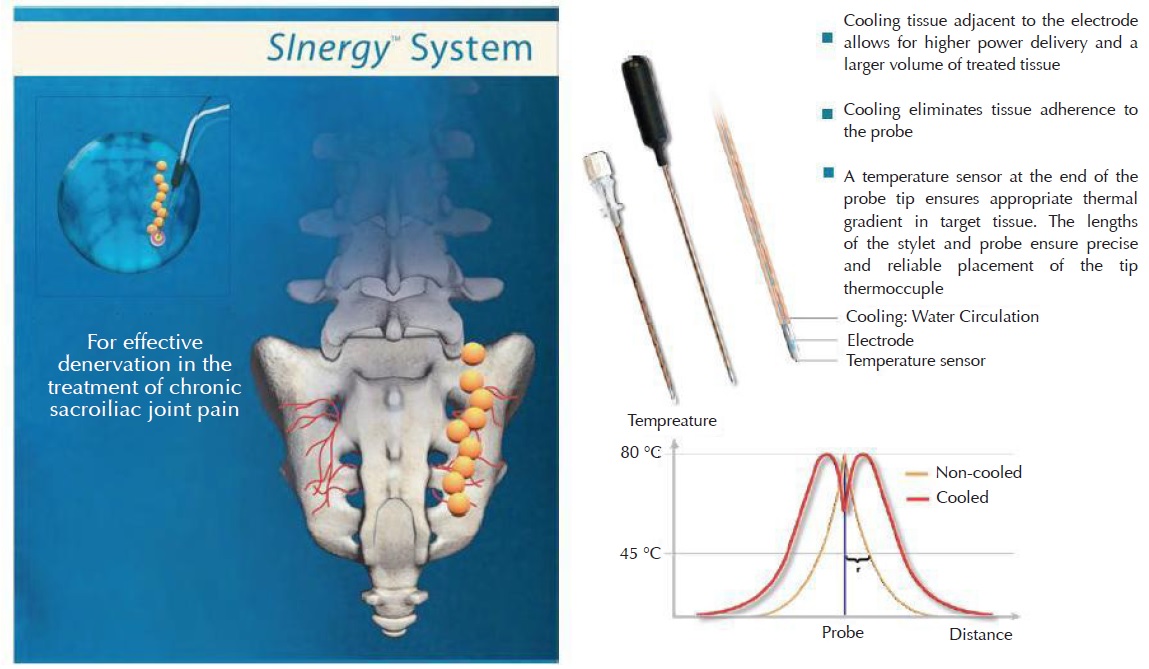
Radiofrequency Denervation Procedures
Radiofrequency (RF) denervation procedures provide prolonged pain relief to patients suffering SI joint pain. The technique is used to denervate the pain fibre supplying the SI joint by creating lesions around the joint. It is a minimally invasive procedure done under local anaesthesia. It is usually day surgery. 2 - 3 puncture holes are made on each side of one SI joint. The surgical risk is negligible. During the RF treatment, a small amount of steroid is given to neutralise the irritation of the RF effect. The treated area will be sore for 1-2 weeks but after that, the pain is significantly reduced. The success rate is 70% [26-28].
|
Surgical fusion of SI joint
The primary indication for SI joint fusion is joint instability or fractures or advanced degeneration. Sacroiliac joint fusion can be done percutaneously by using X-ray or navigation guidance (Fig. 8 and 9). The long-term success rate for SI joint fusion is 70% [29].
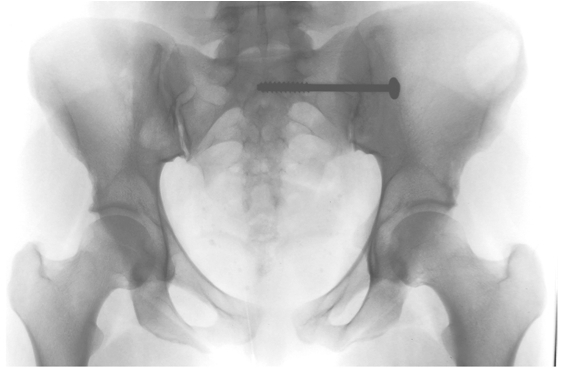 Fig. 8 Anteroposterior radiograph after sacroiliac joint arthrodesis by anterior approach. Ipsilateral iliac crest bone graft was used, followed by transiliosacral compression screw fixation. |
Conclusions
The SI joint is a real, yet under-appreciated pain generator in about 15% to 25% of patients with axial low back pain. Whereas historical and physical examination findings have been previously advocated as useful tools in identifying patients with SI joint pain, more recent studies have demonstrated they have limited diagnostic value. Owing to the complexity of the joint, the mechanisms of SI pain are numerous and ill-defined. If there are no secondary causes (e.g. leg length problem or inflammatory arthritis), local anaesthetic with steroid injection under X-ray guidance is an effective way to confirm the pain origin and at the same time treat the pain. The effect can last for 6 months or longer. One promising area in the treatment of SI joint pain is RF denervation, although there are limited clinical studies. Surgical fusion of SI joint is rarely needed unless there is an obvious instability or advanced arthritis.
Fig. 9 Implants for SI joint fusion. |
References
1. Bernard TN, Cassidy JD. The sacroiliac syndrome. Pathophysiology, diagnosis and management. In: Frymoyer JW, ed. The adult spine: principles and practice. New York: Raven, 1991;2107–30.
2. Dijkstra PF, Vleeming A, Stoeckart R. Complex motion tomography of the sacroiliac joint: an anatomical and roentgenological study [in German]. Rofo 1989;150:635–42.
3. Ruch WJ. Atlas of common subluxations of the human spine and pelvis. Boca Raton, FL: CRC Press, 1997
4. Grob KR, Neuhuber WL, Kissling RO. Innervation of the sacroiliac joint in humans [in German]. Z Rheumatol 1995;54:117–22.
5. Fortin JD, Kissling RO, O’Connor BL, Vilensky JA. Sacroiliac joint innervation and pain. Am J Orthop 1999;28:68–90.
6. Bernard TN, Kirkaldy-Willis WH. Recognizing specific characteristics of nonspecific low back pain. Clin Orthop 1987;217:266–80.
7. Maigne JY, Aivaliklis A, Pfefer F. Results of sacroiliac joint double block and value of sacroiliac pain provocation tests in 54 patients with low back pain. Spine 1996;21:1889–92.
8. Bogduk N. International Spinal Injection Society guidelines for the performance of spinal injection procedures. Part I: zygapophysial joint blocks. Clin J Pain 1997;13:285–302.
9. Dreyfuss P, Cole AJ, Pauza K. Sacroiliac joint injection techniques. Phys Med Rehabil Clin North Am 1995;6:785–813.
10. Dreyfuss P, Michaelsen M, Pauza K, et al. The value of medical history and physical examination in diagnosing sacroiliac joint pain. Spine 1996;21:2594–2602.
11. Elgafy H, Semaan HB, Ebraheim NA, Coombs RJ. Computed tomography findings in patients with sacroiliac pain. Clin Orthop 2001;382:112–8.
12. Maigne JY, Boulahdour H, Chatellier G. Value of quantitative radionuclide bone scanning in the diagnosis of sacroiliac joint syndrome in 32 patients with low back pain. Eur Spine J 1998;7:328–31.
13. Fortin JD, Dwyer AP, West S, Pier J. Sacroiliac joint: pain referral maps upon applying a new injection/arthrography technique. Part I: asymptomatic volunteers. Spine 1994;19:1475–82.
14. Fortin JD, Aprill CN, Ponthieux B, Pier J. Sacroiliac joint: pain referral maps upon applying a new injection/arthrography technique. Part II: clinical evaluation. Spine 1994;19:1483–9.
15. Slipman CW, Jackson HB, Lipetz JS, et al. Sacroiliac joint pain referral zones. Arch Phys Med Rehabil 2000;81:334–8.
16. Dussault RG, Kaplan PA, Anderson MW. Fluoroscopy-guided sacroiliac joint injections. Radiology 2000;214:273–7.
17. Bollow M, Braun J, Taupitz M, et al. CT-guided intraarticular corticosteroid injection into the sacroiliac joints in patients with
spondyloarthropathy: indication and follow-up with contrast-enhanced MRI. J Comput Assist Tomogr 1996;20:512–21.
18. Rosenberg JM, Quint DJ, de Rosayro AM. Computerized tomographic localization of clinically-guided sacroiliac joint injections. Clin
J Pain 2000;16:18–21.
19. Cibulka MT, Delitto A. A comparison of two different methods to treat hip pain in runners. J Orthop Sports Phys Ther 1993;17:172–6.
20. Vleeming A, Buyruk HM, Stoeckart R, et al. An integrated therapy for peripartum pelvic instability: a study of the biomechanical effects of pelvic belts. Am J Obstet Gynecol 1992;166:1243–7.
21. Mooney V, Pozos R, Vleeming A, et al. Exercise treatment for sacroiliac pain. Orthopedics 2001;24:29–32.
22. Lo GH, LaValley M, McAlindon T, Felson DT. Intra-articular hyaluronic acid in treatment of knee osteoarthritis: a meta-analysis. JAMA 2003;290:3115–21.
23. Cohen SP. Sacroiliac joint pain: a comprehensive review of anatomy, diagnosis, and treatment. Anesth Analg. 2005 Nov;101(5):1440-53.
24. Maugars Y, Mathis C, Vilon P, Prost A. Corticosteroid injection of the sacroiliac joint in patients with seronegative spondylarthropathy. Arthritis Rheum 1992;35:564–8.
25. Karabacakoglu A, Karakose S, Ozerbil OM, Odev K. Fluoroscopy-guided intraarticular corticosteroid injection into the sacroiliac
joints in patients with ankylosing spondylitis. Acta Radiol 2002;43:425–7.
26. Cohen SP, Abdi S. Lateral branch blocks as a treatment for sacroiliac joint pain: a pilot study. Reg Anesth Pain Med 2003;28:113–9.
27. Buijs EJ, Kamphuis ET, Groen GJ. Radiofrequency treatment of sacroiliac joint-related pain aimed at the first three sacral dorsal rami: a minimal approach. Pain Clinic 2004;16:139–46.
28. Yin W, Willard F, Carreiro J, Dreyfuss P. Sensory stimulation-guided sacroiliac joint radiofrequency neurotomy: technique based on neuroanatomy of the dorsal sacral plexus. Spine 2003;28:2419–25.
29. Simpson LA, Waddell JP, Leighton RK, et al. Anterior approach and stabilization of the disrupted sacroiliac joint. J Trauma 1987;27:1332–9.
Articles written/edited/reviewed by Doctors of Asia Medical Specialists ©2020 Asia Medical Specialists Limited. All rights reserved. |