Meniscus FAQs Tears Repairs and Transplantation
Meniscus FAQs Tears Repairs and Transplantation
article written by Dr CC KONG
(Last updated on: Oct 13th 2020)
What is a meniscus?
The menisci are two rubbery crescent moon shaped flat pieces of cartilage in each knee (Fig. 1). The English colloquial term is 'cartilage', which can be confusing because the knee also contains articular cartilage, the smooth covering of the bone ends which makes a joint a joint rather than two pieces of bone rubbing together. The Chinese colloquial term 'half-moon-shaped flat plate of cartilage' (半月板) is very descriptive. The main purpose of the meniscus is to act like a washer – spreading load – in this case load on the articular cartilage.
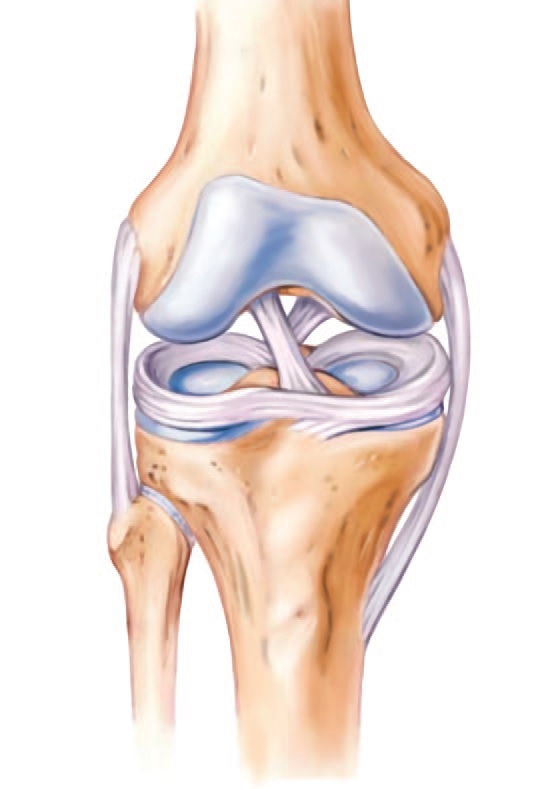 Fig. 1 half-moon-shaped flat plat of cartilage |
How do menisci get torn?
A violent injury like a ski accident or fall can tear a meniscus, but, because the menisci live in a very harsh environment, and are subjected to huge forces in everyday life, the menisci can tear simply standing up from sitting or climbing a step. As one gets older the menisci degenerate and soften, a bit like cheese ripening, and they can tear very easily.
What will happen to my knee if my meniscus is torn?
If the tear is small and stable it may heal on its own. If the tear is larger or unstable it will most likely spread and become more serious. If a meniscus is removed or severely damaged the knee will develop arthritis. Before arthroscopic surgery was developed in the 1970s the only treatment for a meniscus tear was to remove the meniscus. Young people usually developed pain from arthritis 15 – 20 years later – and by this time their arthritis was already advanced [1]. If one only has a small part of the meniscus damaged or removed the problem will not be as severe.
"…if a meniscus is removed or severely damaged the knee will develop arthritis."
How do I know if my meniscus is torn?
The diagnosis is best made by Magnetic Resonance Imaging (MRI), which is about 95% accurate for meniscus tears. MRI shows the tear (Fig. 2), but it cannot usually show whether the meniscus is likely to heal on its own, needs an arthroscopic (keyhole) surgical repair, or is unrepairable. The only way to be sure is to have an arthroscopy (Fig. 3).
"MRI is about 95% accurate for meniscus tears"
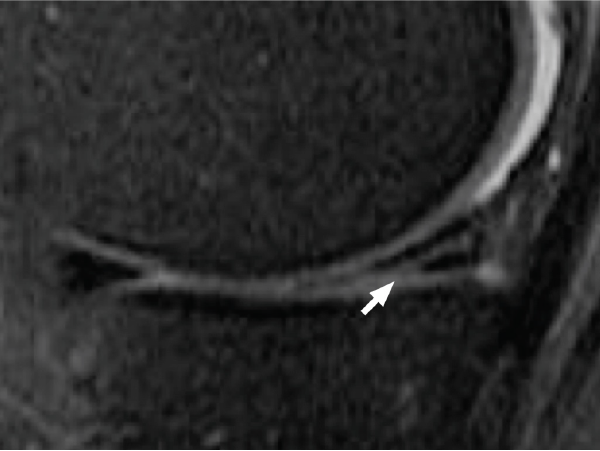 Fig. 2 MRI shows a meniscus tear - the arrow points to a white line in the black triangle of the meniscus |
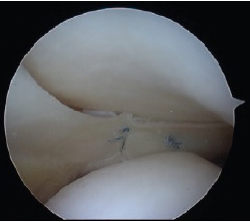
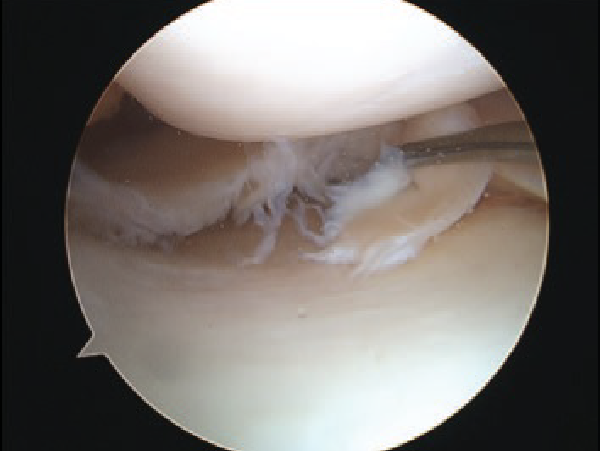 Fig. 3 Arthroscopic view of the meniscus tear |
What should I do if my meniscus is torn?
The modern answer is 'have it repaired if possible'. Asia Medical Specialists offer the latest techniques of arthroscopic meniscus repair in Hong Kong, Beijing, Shanghai and Guangzhou. One has an epidural or general anaesthetic, and the procedure takes up to about one hour. It is a minimally invasive procedure with tiny incisions, so one can walk the same day, and though it can be sore, it is not usually painful. Most people go home from hospital the same day or the next morning, and return to office jobs after 3 or 4 days. If one is lucky, the meniscus tear will be found to be small and stable, and likely to heal on its own. If one is not quite so lucky, the meniscus will need repairing, and one will have to protect the repair (no running for 2 months and no squatting or twisting for 3 months).
If one is unlucky the meniscus will not be repairable and will need to be trimmed. On the bright side, recovery from meniscal trimming ('meniscectomy') is usually very quick, and many people are 90% recovered after a week or two. For all these procedures, Asia Medical Specialists have rehabilitation protocols for one to follow with one's physiotherapist. Unfortunately, none of these procedures is 100% reliable, as the meniscus lives in a very harsh environment – it is subjected to huge loads, even if one is careful, and does not have a very good blood supply, which reduce its healing ability. Small tears may fail to heal, meniscus repairs may fail, menisci that have been trimmed may develop fresh tears, all of which would mean a repeat operation.
“…have the meniscus repaired if possible”
What if a significant portion of my meniscus has been removed?
Depending on one's age, one should consider some sort of replacement, in the hope of preventing future arthritis. Broadly, there are two options available in Hong Kong: 'Regeneration' and 'Transplantation'. Regeneration is simpler, but is not suitable for the most severe meniscal loss.
What is 'meniscal regeneration'?
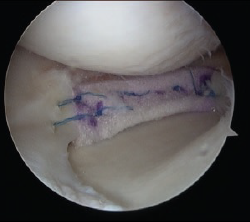
In the technique used by asia medical specialists in Hong Kong, essentially a meniscus-shaped sponge is stitched into the gap in the meniscus arthroscopically. The body’s own meniscal cells inhabit the sponge, and gradually secrete collagen, turning it into a new meniscus. Short term results are excellent – most people have relief of any pain – but the procedure is too new for us to know if it will prevent arthritis in future.
Asia Medical Specialists performed the first operation of this type in Hong Kong in 2013, and use the Actifit™ meniscal scaffold, made by Orteq Bioengineering of London, UK. The Actifit received CE Mark European Accreditation in 2008 . The Actifit is made of polyurethane and has been shown to be a safe, effective implant, for the treatment of patients with pain as a result of segmental medial meniscus loss at 2 years.
a meniscus scaffold regenerates meniscus tissue
If the meniscus lost completely, a meniscus transplant may be a better option to replace the missing meniscus. Meniscus transplantation involves taking a size-matched meniscus from a donor and stitching it into the recipients' knee. The donor is carefully screened for contamination, and if the contamination-test results are clear, the tissue is provided to surgeons for transplantation. The menisci that Asia Medical Specialists use are provided by the Musculoskeletal Transplant Foundation in the USA, and their record on contamination is excellent. The operation is performed arthroscopically. The menisci are not rejected, so no drugs are needed. The procedure is relatively new, so, although we know that the transplanted menisci remain in the knee, and look like normal menisci, we do not yet know whether they function like normal menisci to prevent arthritis, though it seems likely they will.
"a meniscus transplant replaces the missing meniscus"
 | 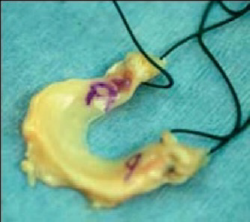 |
Meniscus Transplant | |
|  |
| Meniscus scaffold for meniscus regeneration | |