Trigger Finger-causes, symptoms and treatments
Trigger Finger(stenosing tenosynovitis) – causes, symptoms and treatments
reviewed by doctors of Asia Medical Specialists
(Last updated on: May 3rd 2021)
Have you ever experienced one of your fingers stuck in a bending position? When you try to straighten it, it comes with a snap? Or sometimes, when you woke up, you noticed one of your fingers is bent and can't straighten up…….?. You might have a "trigger finger".
What is a Trigger finger?
Trigger finger is a painful condition that usually appears between the ages 40 and 60[1]. Once you try to bend your finger, the digit will be locked. The formal medical name of trigger finger is called "stenosing tenosynovitis". In the cases when your thumb is experiencing such symptoms, it is called "trigger thumb".
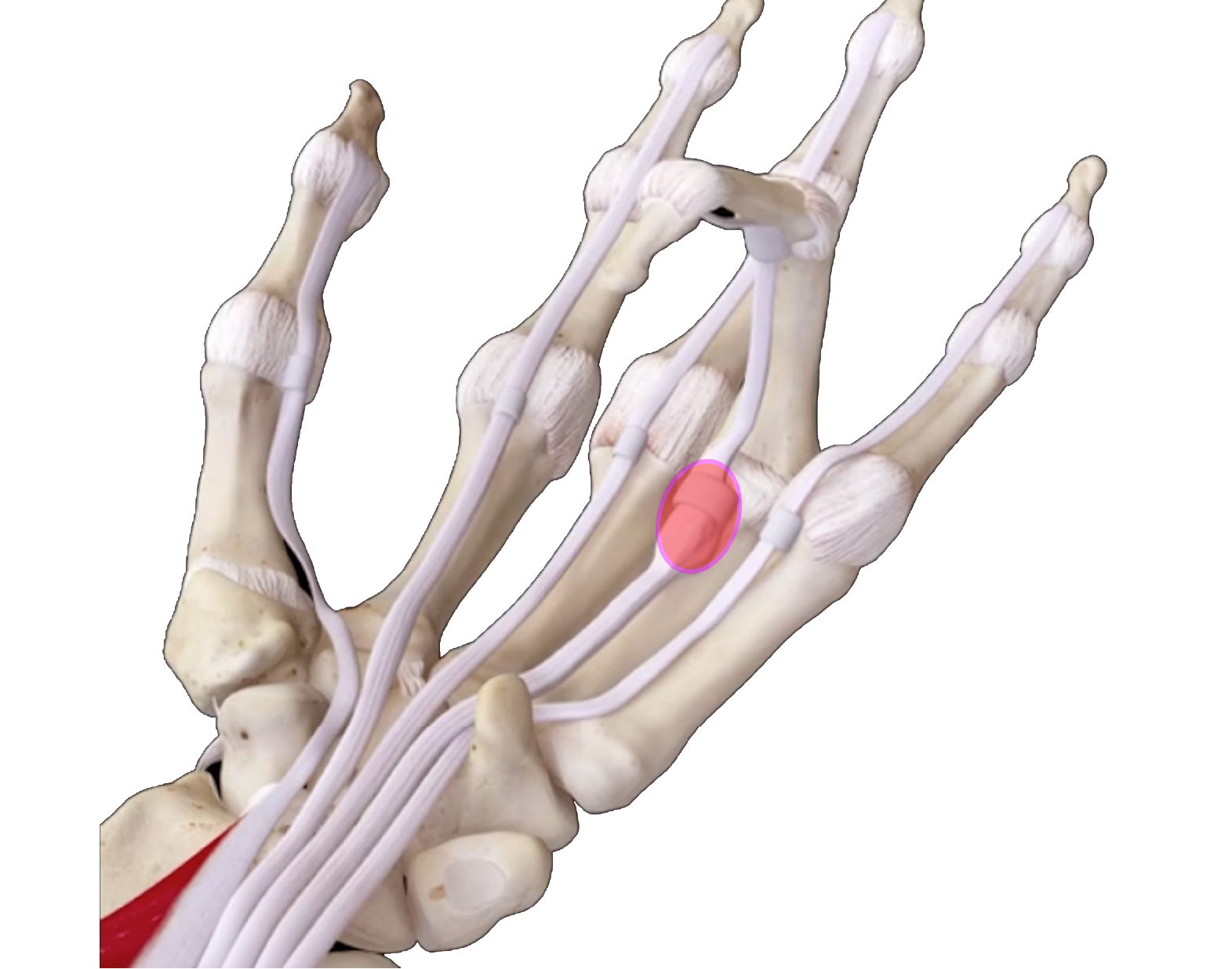 |
| Fig 1. Trigger Finger |
Trigger finger symptoms
In the early stage, the symptoms of trigger finger usually are mild and not that obvious.
Following are some of the common signs that a person may experience:
- "clicking" sound when bending and straightening the finger or thumb
- The patient will experience pain and thickening(nodule) at the base of the thumb or finger.
- Under some circumstances, the finger will be "locked" and can't be straightened.
- Stiffness of the finger, especially in the morning.
Based on the severity, trigger finger can be classified into four stages (The Green Classification)[2]
| Stage I | Inflammation on AI pulley with swollen and pain |
| Stage II | The patient can still straighten the finger, but with "catching" of the digit |
| Stage III | The affected finger need external forces to straighten the finger |
| Stage IV | Fixed flexion contracture of the finger joint (Proximal interphalangeal joint |
Trigger finger risk factors and causes
It is believed that the cause of the trigger finger is due to a repeated movement of the finger/thumb, causing degeneration of the flexor tendon and thickening of the A1 pulley.
Such thickening affects the tendon motion. When the person tries to bend his/her finger, this pulls the inflamed tendon through a narrowed sheath that makes the snap or pop.
- Age: Trigger fingers happens between age 40 and 60 (sometimes younger or older)
- Health Conditions: Diabetes patients or people who are suffering from rheumatoid arthritis or gout.
- Work: It is also common to find that people use their finger/thumb in a repetitive movement during work or play to develop Trigger finger. Pianist, or farmers
- Surgery for carpal tunnel syndrome:Usually, this is common during the first six months after the operation[3]
Trigger finger diagnosis
The diagnosis of trigger finger is pretty straight forward; there is no need for X-rays or Lab test. The doctor will usually do a physical exam on your hand and finger by asking the patient to open and close the hand and perform other movements and symptoms that the patients described.
Different Diagnosis
One of the main characteristics of a trigger finger is the "locked" symptoms; however, such a characteristic is not unique to just a trigger finger. Other problems associated with a locking (Deformed) digit could be Dupuytren's Contracture. If the complaint of the pain is at the MCP joint (Thumb), this could be related to:
- De Quervain's syndrome (Mommy's Thumb)
- Skier Thumb
- MCP joint sprain
Trigger finger Treatment
Non-invasive treatment
REST
Trigger finger treatment is not complicated and depends on the severity of the conditions; the doctors will usually ask the patients to start with getting a rest. Stop doing things that might worsen the condition
Injection
A Lot of people are responsive to Steriod injection on the inflmated joint. Usually patients enjoying symptom relief two years after injection are likely to maintain long-term success.
Exercises
Based on the patient condition, the doctor would sometimes recommend the patient conduct stretching exercises that would help ease some of the stiffness. Exercising also can improve the range of motion within the thumb and fingers.
Surgery Treatment
If non-invasive treatments fail to improve the condition, your doctor would consider conducting an A1 pulley release procedure. Such a procedure can be performed either by a surgical incision or piercing the skin with a needle performed under local anaesthesia as an office procedure.
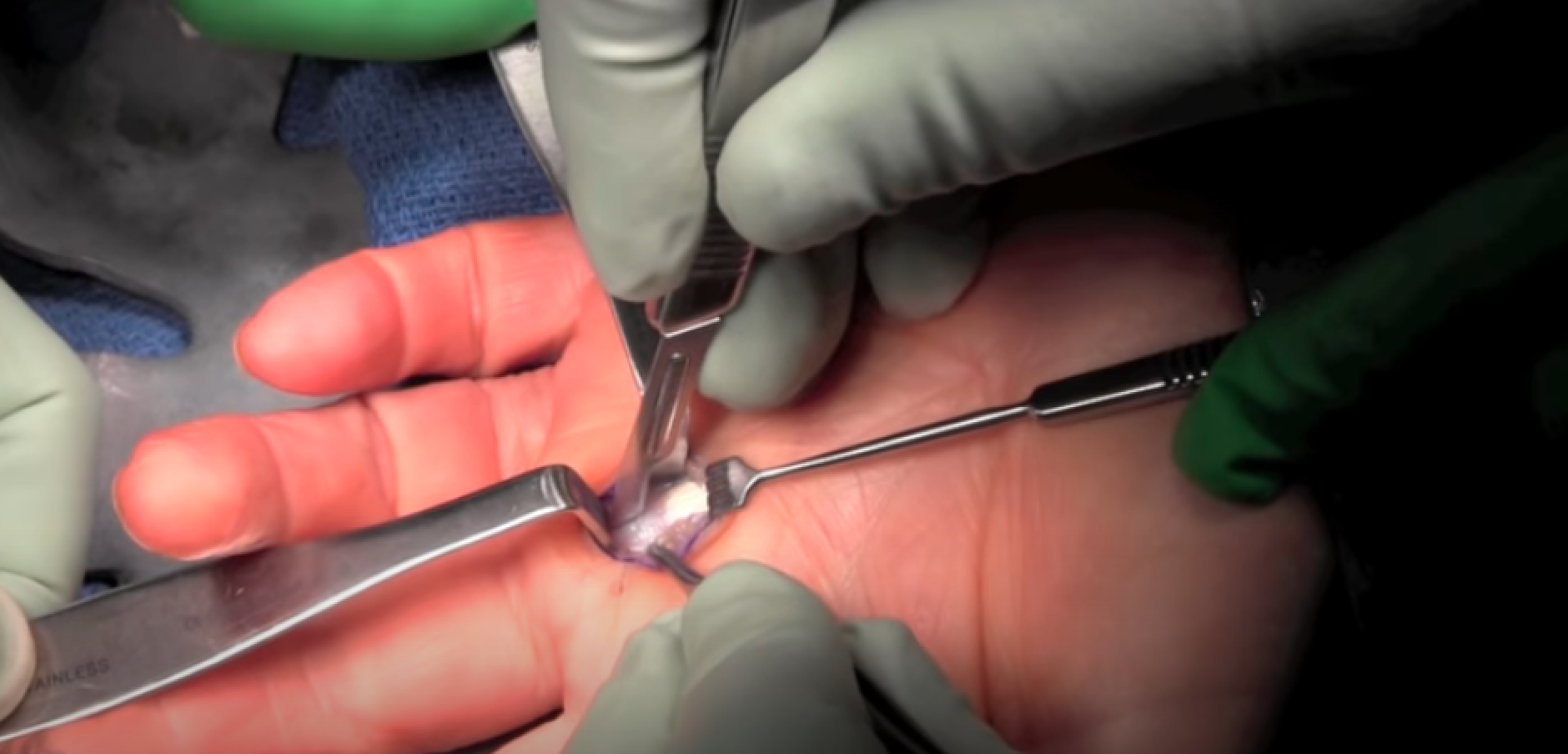
Surgical AI pulley release
This procedure is quite simple and straight forward.
- The surgeon will administer local anaesthesia.
- A small incision will be made in the palm.
- The surgeon will then locate the tendon sheath restricting the movement and carefully cut through it to make way for the tendon to slide.
- Before closing up the incision, the surgeon may try to flex and extend the finger/thumb to see if the tendon has enough space to move freely.
 |
[1] Trigger Finger, Harvard Health Publishing, Harvard Medical School, May 2015
[2] The Efficacy of Steroid Injection in the Treatment of Trigger Finger
[3] Trigger Finger, Trigger finger risk factor, webMD August 24th, 2020
