Hamstring Tendon Tears FAQs
Hamstring Tendon Tears FAQs
Written By Dr Jason BROCKWELL
(Last updated on: Oct 13th 2020)
What is this article?
This provides information to patients on proximal hamstring tendon ‘tears’ or ‘bone avulsions’, but not ‘tendinitis’ or ‘tendinopathy’.
Proximal means the part of the hamstring tendon that attaches to the ischial bone in the pelvis. These are also known as ‘high’ hamstring problems.
A ‘tear’ in this context usually means the tendon tears away from the bone. Sometimes the tendon pulls a piece of bone away, instead of tearing away from the bone, and this is called a ‘bone avulsion’. The ‘Hamstring Tendinopathy FAQs’ describe ‘tendinitis’, which is usually treated differently.
How are hamstring tendons diagnosed?
Usually people have a pain and ‘snap’ or ‘pop’ in one buttock during sport. Typically the knee is straight and the hips bent at the time, which tensions the hamstring muscles. The classic description of the injury is in water skiers, but it can occur in almost any sport – for example stepping on a tennis ball during a rally or losing one’s balance doing the splits in Yoga, or being ‘jack knifed’ in a Rugby scrum.
Sometimes a person has chronic pain from ‘tendinopathy’ and the tendon pulls away from the bone unnoticed, or as a result of an injury that is the final insult to a damaged tendon. Physical examination often shows:
1. A positive ‘bowstring test’ – there is reduced tension in the hamstring tendons behind the knee [1].
2. Tenderness of the tendon in the buttock.
3. Pain and weakness on resisted hamstring contraction.
4. Depending on the timing, there may be bruising of the thigh.
5. Sometimes one can feel the torn tendon end in the back of the upper thigh.
X-ray is normal if the injury is to the tendon, but will be abnormal if there is an avulsion fracture.
MRI shows the tendon pulled away from the bone and surrounded by blood or scar tissue.
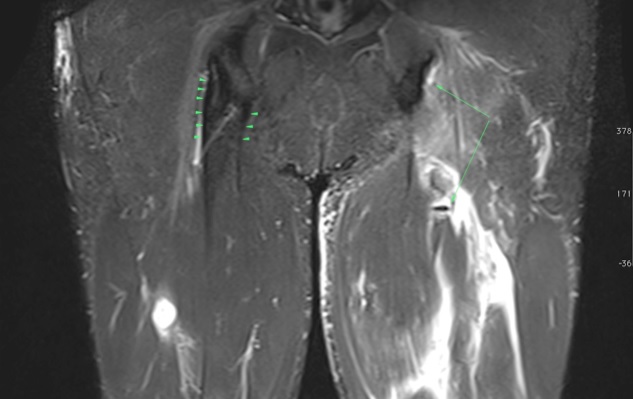 MRI shows normal tendon on the right (arrowheads) and absent tendon on the left. The upper long arrow points to where the tendon should be, and the lower long arrow points to the loose end of the tendon – seen as a short black line, sitting in the upper thigh. |
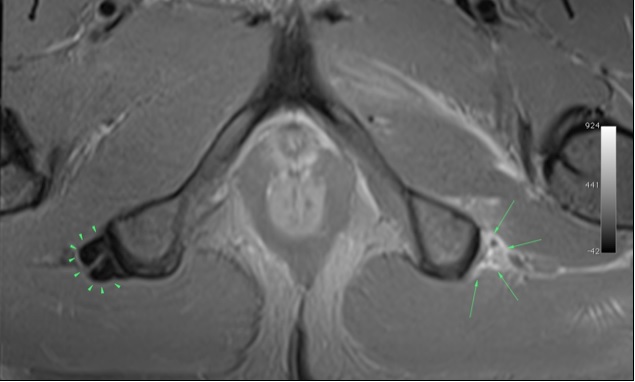 MRI shows the normal appearance of the hamstring tendon on the ischial bone on the right (arrowheads) and absent tendon on the left (arrows). |
What is the treatment of hamstring tendon avulsion fractures?
If a new fracture is ‘undisplaced’ – meaning that if it heals in that position everything will be fine, no special treatment is needed. If a new fracture is displaced (i.e. pulled out of its normal position), it is best treated by an operation to fix the fractured bone back in the normal position, usually with screws.
If the fracture is old, and has failed to heal, and there are symptoms, it is best treated by an operation to fix the fractured bone back in the normal position, usually with screws. If the fracture is old and there are no symptoms, there is no need for any treatment.
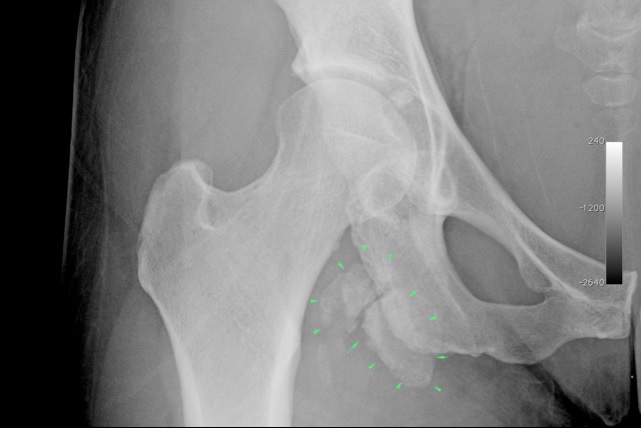 X-ray shows old unhealed avulsion fractures of the origin of the hamstring tendons (arrows). There were no symptoms, so no treatment was required. |
What is the treatment of hamstring tendon tears?
The proximal hamstrings have slightly complex anatomy – there are 3 muscles, but only 2 tendons, because the tendons of two of the muscles join together to form one ‘conjoint’ tendon.
Single tendon avulsions with less than 2cm gap may recover well if the torn tendon heals to its uninjured fellows.
A significant gap usually means all three tendons are torn or a single tendon has torn with associated injury to the surrounding muscles. Although the incidence of this injury is unknown, as it is not easy to diagnose without MRI or ultrasound, the consensus in the medical literature is that early surgical repair is the best treatment [2].
Chronic ruptures with symptoms should be repaired, as they will improve with surgery [3], but generally do not do as well as early repairs, and the risk of damage to the sciatic nerve is higher.
Chronic ruptures without symptoms do not require treatment.
What is the best time for an operation? Can I wait and see how I get on, and have operation later if needed?
If the injury is recent and meets the above criteria for surgery, it is best to have the operation within about 3 weeks of the injury, as, with more time, scar tissue forms, making the operation more difficult. This only matters because the scar tissue may involve the important sciatic nerve, which supplies power and sensation to the lower leg, and which runs next to the hamstring tendons. Sciatic nerve damage can be a very severe problem, so it does make sense to have the operation earlier.What is the best time for an operation? Can I wait and see how I get on, and have operation later if needed?
If the injury is old, it does not matter much when the operation is performed.
How is a hamstring tendon repair operation performed?
The operation is performed in hospital with a general or regional anaesthetic. The patient lies face down on the operation table. An incision is made in the infragluteal fold (the crease under one’s buttock – so usually the scar is hidden). The incision is usually about 7 - 8cm long. The hamstring tendons and ischium are exposed and mobilised (freed of any scar tissue). If scar tissue involves the sciatic nerve, which lies next to the tendons, it may need to be released. The avulsed bone fragment or the torn tendon is repaired. Bone fragments are usually fixed with screws and the tendons are usually reattached to the bone using special anchors with Kevlar sutures.
What is the recovery?
One needs to walk with the aid of crutches for balance for up to six weeks. Initially most of one’s weight goes through the crutches, with the leg just carrying it’s own weight, but, as it feels stronger, one can put more weight through the leg, using the crutches just for balance, then using only one crutch (in the hand on the opposite side to the operated leg), and then abandon support entirely when the leg has regained its strength – which usually
takes 4 to 6 weeks.
How long will I need to be in hospital?
One can leave hospital as soon as one is able to get around safely and independently – i.e. able to use the bathroom, get up and down stairs and get in and out of a car. Most people leave hospital the day following their operation or the day after that.
Do I need a brace?
It is probably not necessary to use a brace postoperatively as the muscle does not contract until the repair is secure (at 6 – 8 weeks) and the body ‘protects itself’. (There are no scientific studies on brace vs no brace or any other aspects of post-operative rehabilitation.) One should avoid bending the hip while the knee is straight e.g. sitting with ones feet up, but it is safe to lie propped up in bed to read or work on one’s laptop.
Is physiotherapy needed?
Physiotherapy is very helpful, and most people go to their physiotherapist regularly until they are well on their way to recovery – usually once or twice a week for a month and then once a week or once a fortnight for another two months (i.e. a total of about 3 months). It takes a good six months to recover 90%.
References
1. Birmingham, P., et al., Functional outcome after repair of proximal hamstring avulsions. J Bone Joint Surg Am, 2011. 93(19): p. 1819-26.
2. Harris, J.D., et al., Treatment of proximal hamstring ruptures - a systematic review. Int J Sports Med, 2011. 32(7): p. 490-5.
3. Cross, M.J., et al., Surgical repair of chronic complete hamstring tendon rupture in the adult patient. Am J Sports Med, 1998. 26(6): p. 785-8.
| Copyright ©2017 Asia Medical Specialists Limited. All rights reserved. |
